PRAM fits a unique niche in the health benefits marketplace. This page should give you an overall view of what we do.
What is PRAM’s Role?
PRAM serves as the hub for managing and servicing your prescription program. PRAM contracts with the PBM and Carrier to bring you the best possible plans for your membership base. PRAM:
- Develops & underwrites national pharmacy benefit programs
- Manages implementation, billing, and enrollment
- Manages eligibility and claims management
- Manages Distribution Partner, Plan Sponsor, Carrier, & PBM relationships
- Provides financial management and reporting
- Audits pharmacy claims
- Provides advice for cost-containment strategies
- Prepares and files policies with state entities

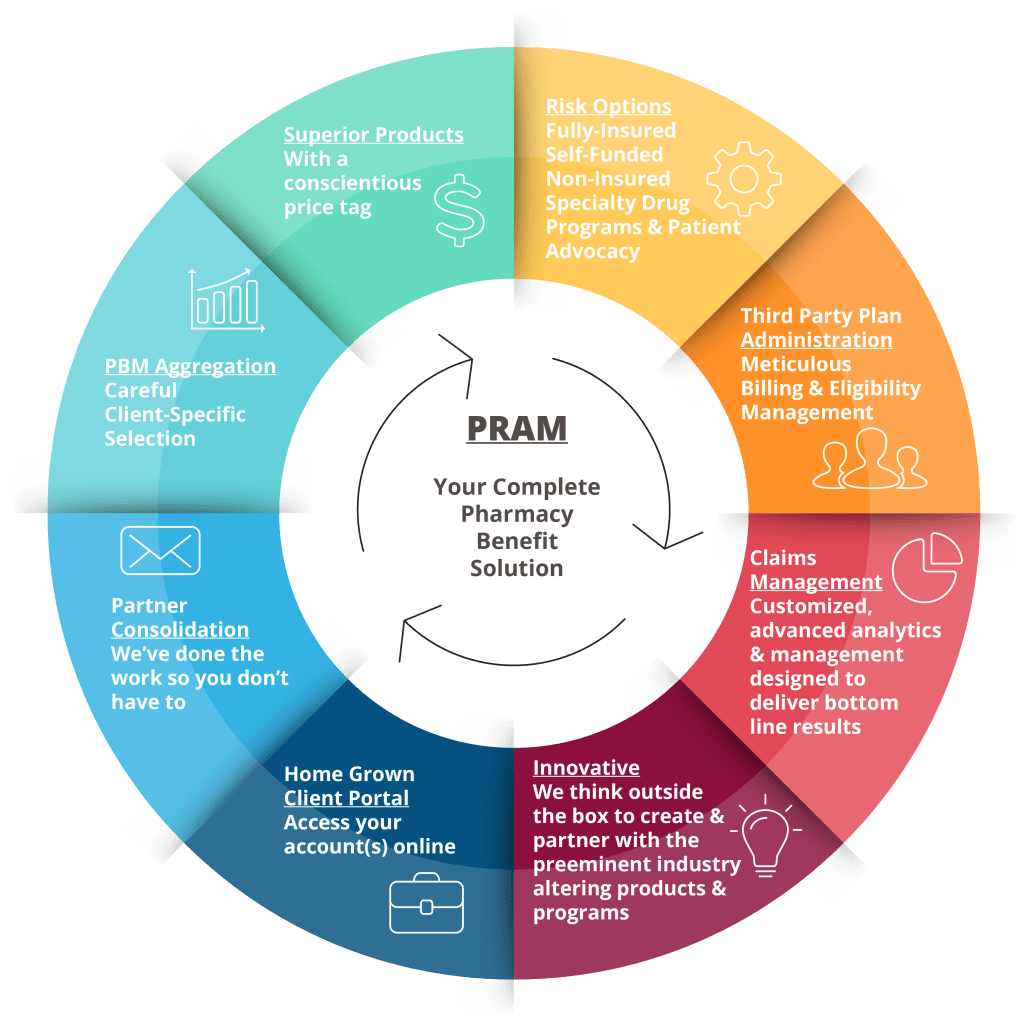
PRAM Services
Management of your Prescription Benefits just got so much easier with PRAM.
Since 1989, PRAM has established itself as a trusted leader and industry expert, specializing in prescription drug solutions. Our clients, who come from every corner of the industry, rely on us for comprehensive consulting and benefit management services. Whether it’s navigating complex benefit structures or optimizing drug plans, we provide tailored solutions to meet diverse needs. Our expertise spans a wide range of parameters, as illustrated in the graphic to the left while always ensuring that we deliver the highest level of service and value to our clients.


